Paul Mulholland speaks to HSE national antimicrobial resistance and infection control team member Ms Mary McKenna about the importance of hand hygiene in the Covid-19 era
Knowledge about the benefits of proper hand hygiene etiquette is at a societal and cultural high point as a result of the Covid-19 pandemic. In recent months, public health specialists, other experts, and politicians across the globe have repeatedly highlighted how washing your hands in a thorough manner is a vital means of stopping the spread of infection.
Of course, healthcare professionals have been aware of this for some time in the context of preventing healthcare-associated infections. In recent years in Ireland, there had been increased focus on hand hygiene in healthcare settings, with acute hospitals having to agree to hand hygiene audits using the national protocol since 2011.
In 2013, the HSE issued a memo stating that all healthcare staff should receive mandatory hand hygiene training on induction and at least every two years. Then in 2017, the HSE’s Hand Hygiene Train the Trainer programme (which is part of the RESIST programme) was rolled-out in community settings, and later across Hospital Groups.
Ms Mary McKenna is Assistant Director of Nursing, Infection Prevention and Control, and a member of HSE national antimicrobial resistance and infection control team. Speaking to the Medical Independent (MI), Ms McKenna said that the Train the Trainer programme has essentially served to “pre-prepare” the health system for Covid-19 by embedding good hygiene practice across the community and acute settings.
Community
The origins of the Train the Trainer programme lay in a deficit of community infection control nurses, which was identified in a gap analysis. The programme was created to provide education, guidance and tools to enable other healthcare workers to deliver hand hygiene training in their service.
“There is an acknowledged deficit that you have with community infection control nurses because the geographic spread is very vast,” according to Ms McKenna.
“In some areas, you may have had a support from a community infection control nurse to all services, but in other areas, there may just have been one community infection control nurse. It would be very challenging for her to reach out with a programme of hand hygiene education to teach individual services to deliver face-to-face training to all of the staff.
“By having the trainers on board, she or he was in position to skill-up and to spread the knowledge and the learning by having trainers doing that in individual facilities so that it was a better and efficient use of their resource capacity and their expertise.
“With the deficit in community infection control nurses and looking at what was actually taking place across the various community services, we noticed there were pockets of good practice. So for example, in Cork, Kerry, and Donegal, they had some small-scale hand hygiene training and assessment projects undertaken that seemed to have some merit. So we developed a template that would create a standardised approach nationally for training across all the Community Healthcare Organisations (CHOs).”
Training materials were developed to support healthcare workers’ competency in delivering safe care with mandatory hand hygiene education.
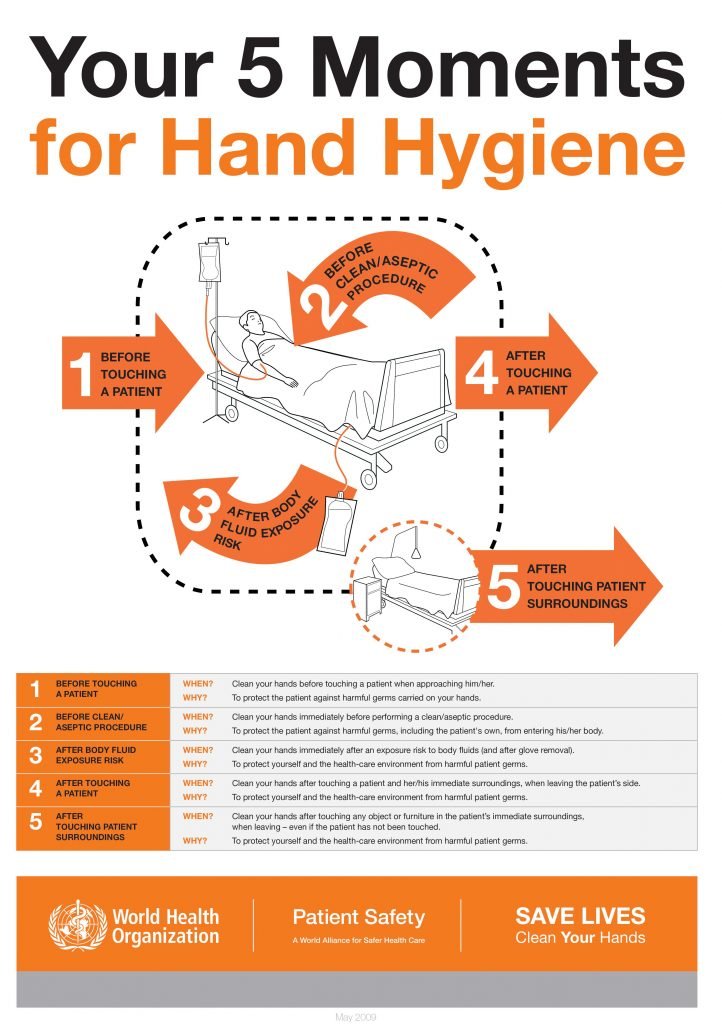
Central to good hygiene practice in a healthcare setting, according to Ms McKenna, is the World Health Organisation (WHO) ‘five moments’ approach (see illustration).
“We went out and delivered programmes to pretty much all of the CHOs and this was supported with the community infection control nurses,” Ms McKenna said.
“They went on to deliver the trainer programme themselves locally to trainers. So you had a domino effect of bringing the frontline more aligned with standardised approach, but having that local person, who is going to be a champion in their workplace. We had about 850 hand hygiene trainers trained across all of the community. We monitored to a certain degree, and they were asked to do returns of how many staff were training in which areas. So by 2019, we knew that over 14,000 staff had availed of hand hygiene education using this approach.”
Hospitals
In 2018, there was an interest from the acute hospitals to have a similar approach developed. The following year a pilot programme was established, which included: University Hospital Limerick; Portiuncula University Hospital, Ballinasloe; Cavan General Hospital; and the National Maternity Hospital, Holles Street. Since then, the programme has been rolled-out to other hospitals. Training was tailored depending on the areas in which staff worked. Ms McKenna acknowledged that hospitals are busy environments, which can make it challenging for staff to take the time to follow correct hand hygiene protocols.
“Where you have a very busy environment and where you have a shortage of staff and time is a factor, there may be a lesser practice of hand hygiene than if there was time available,” she said.
“So as part of training, we highlighted to staff to prioritise the importance of hand hygiene for each of their care activities so that hand hygiene is seen as one of the key important measures in place to prevent healthcare-associated infections.
“We say to staff on the day they attend the training, ‘what are the most important priorities in a busy environment?’ We look at how hand hygiene can be built in as one of those priorities. Part of our quality improvement exercises given to staff was, how do you give someone an infection, and actually getting people to look at the negative things that can happen by not cleaning your hands, wearing gloves and not changing them, and then seeing, can any of these be corrected? Whilst staff are really busy and have other activities to attend to, it’s important that healthcare-associated infection is really up there in terms of their priorities.”
CPE
Before Covid-19, the spread of carbapenemase-producing Enterobacteriaceae (CPE) in healthcare settings warranted the calling of a public health emergency. Correct hand hygiene practice plays an important role in controlling the spread of CPE and has been a central focus of the Train the Trainer programme, according to Ms McKenna.
“CPE was a focus of our work at that particular time; it was an example of bringing hand hygiene to real life, supporting the public health emergency which still prevails,” she said.
While Covid-19 now assumes top priority, Ms McKenna said “CPE still remains a challenge and transmission of CPE still remains a priority as well”.
Impact of Covid-19
Ms McKenna said it was beneficial that the programme was up-and-running before the Covid-19 pandemic. Although training is no longer taking place in person, the use of online resources, including webinars, allows staff to continue to receive updates on best practice. Also, the protocols taught in the programme play an important role in the correct use of personal protective equipment (PPE).
“I’m very assured that in all hospitals since the Covid preparedness began, that hand hygiene education has been built into that,” Ms McKenna told this newspaper.
“While staff haven’t been doing a specific Hand Hygiene Train the Trainer programme outreach, they have been embedding hand hygiene as a very key part in the use of the personal protective equipment.
“Every healthcare worker in acute hospitals needs to understand personal protective equipment and in doing so, they need to know how to perform hand hygiene. I believe that the awareness around hand hygiene has increased with the need that was put in place with preparedness for Covid-19 and certainly the hand hygiene train the trainer programme was in no way lost.”
Ms McKenna pointed out that acute hospital audit data on hand hygiene practice in December 2019 found 92 per cent compliance with best agreed protocols, which was just above the HSE target of 90 per cent.
Since then, awareness of the importance of hand hygiene has only increased.
“I do believe that there has been significant awareness around the practical importance of hand hygiene in everything we do, both within hospitals and healthcare facilities and among staff,” she said.
“Everyone sees hand hygiene as the priority at the moment because of Covid-19. The advice is, the top things that you can do are: Stay at home; no unnecessary travel; no unnecessary activities; clean your hands. As well as within the healthcare facilities, when you go into shops or open premises at the moment, the first opportunity to engage within that facility is to use an alcohol hand gel dispenser. Certainly, it will drive hand hygiene to its rightful place in the prevention of transmission of all infections going forward, currently within the pandemic, but also I believe it will be a high priority in our future lives.”



